The Orthopedic Specialty Clinic at TOSC
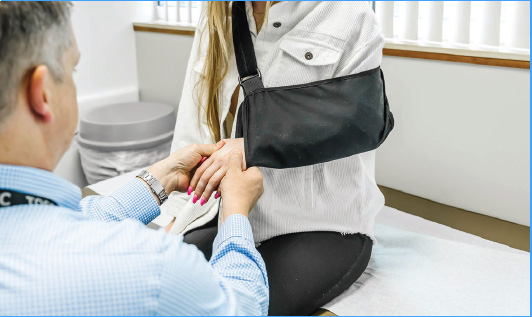
Our Orthopedic Specialist excel in providing the highest level possible of service to those with musculoskeletal needs. Our board-certified and fellowship trained staff are highly specialized in their areas of expertise and work together to provide the best possible outcomes for their patients.
The Orthopedic Specialty Clinic offers the highest level of surgical services including advanced total joint replacement using state-of-the-art equipment and techniques. Whether your surgery is outpatient or requires an overnight stay our friendly staff is there for you.
-
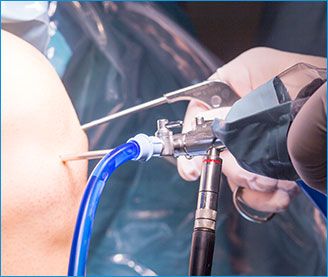
Sports Medicine, also known as sports and exercise medicine (SEM), is a branch of medicine that deals with the treatment.
-
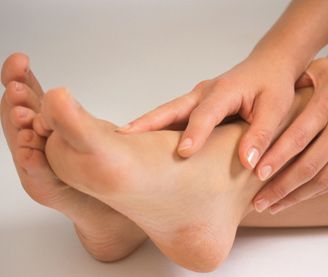
Common foot and ankle injuries include sprains, strains, ligament or tendon tears, and bone fractures. Depending on the diagnosis, appropriate non-surgical or surgical treatments will be used to restore mobility and function in the foot and ankle.
-
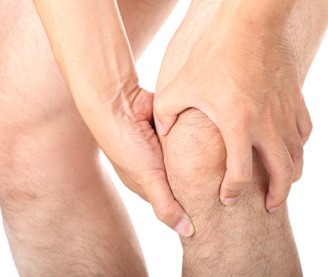
General Orthopedics involves the comprehensive and coordinated care of a wide range of musculoskeletal conditions ranging chronic arthritis to acute bone and joint injuries. Treatments are customized to meet the needs of the patient.
-
Hands are our interface with the world. As a result, hand injuries are common, and can drastically affect day-to-day life. Function of the hand is dependent on precise interaction of the many bones, tendons, nerves, and blood vessels that compromise the human hand. These structures allow us to care for our children, complete a day’s work, or enjoy our pastimes and passions.
-
Joint replacement is a surgical procedure in which the worn, damaged surfaces of the joint are removed and replaced with new artificial parts. Your doctor may consider a joint replacement if you have severe pain which limits daily activities and is not relieved with medications, injections, physical therapy, or other treatments.
-
Trauma and fractures are acute injuries that cause significant pain and discomfort. Treatment depends on the severity of the injury and includes medication, setting of the bone, immobilization, physical therapy, and surgery.
-
TOSH Research efforts focus on performance enhancement methods and protocols, injury risk reduction,

We are located in the South East blue parking lot. Entrance #3 shown in Blue is the closest parking to our clinic